Tras haber chocado su bicicleta contra una barrera, Katie Zaferes...
Leer más
Higher Mortality for Acute CVD Conditions at Rural U.S. Hospitals
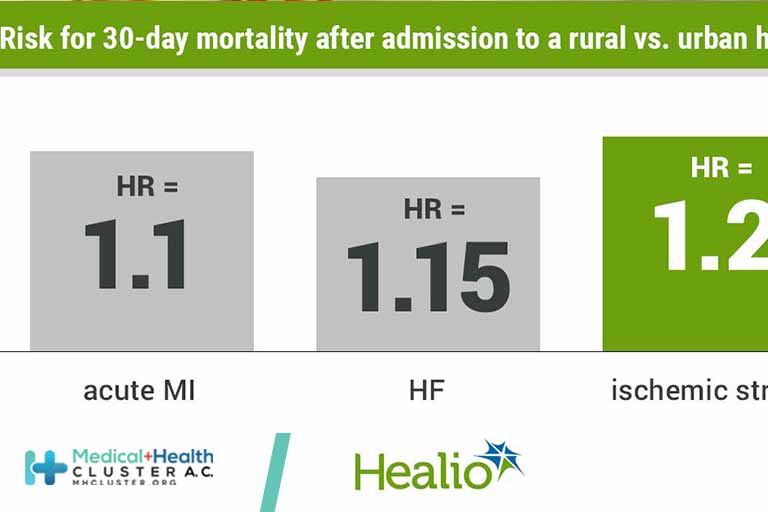
Use of potentially beneficial therapeutic procedures was also lower at rural hospitals than at urban ones.
Rural-urban health inequities have been previously documented. To evaluate rural-urban disparities in outcomes of acute myocardial infarction (AMI), heart failure, and ischemic stroke, authors performed a retrospective analysis of data from over 2 million Medicare beneficiaries hospitalized for these conditions between 2016 and 2018.
After adjustment for demographics and comorbidities, 30-day all-cause mortality risks were significantly elevated by 10% to 20% among patients presenting to rural hospitals with AMI, heart failure, or ischemic stroke compared with those presenting to urban hospitals. Patients at rural hospitals were also significantly less likely to undergo important therapeutic procedures than patients at urban hospitals. These included cardiac catherization (received by 50% vs. 64% of patients at rural vs. urban hospitals, respectively), percutaneous coronary intervention (42% vs. 46%), and coronary artery bypass graft (9% vs. 10%) in AMI patients, and thrombolysis (3% vs. 10%) and endovascular therapy (1.8% vs. 3.6%) in patients with ischemic stroke.
Among rural hospitals, mortality rates were markedly higher and procedural rates markedly lower among the critical access hospitals that serve more-remote areas.
https://www.mhcluster.org/2022/02/07/novavax-covid-jab-approved-by-mhra/
Créditos: Comité científico Covid