En atención a la creciente preocupación sobre la confianza en...
Leer más
Home Pulse Oximetry for COVID-19 in Low-Resource Settings: Undervalued and Underutilized?
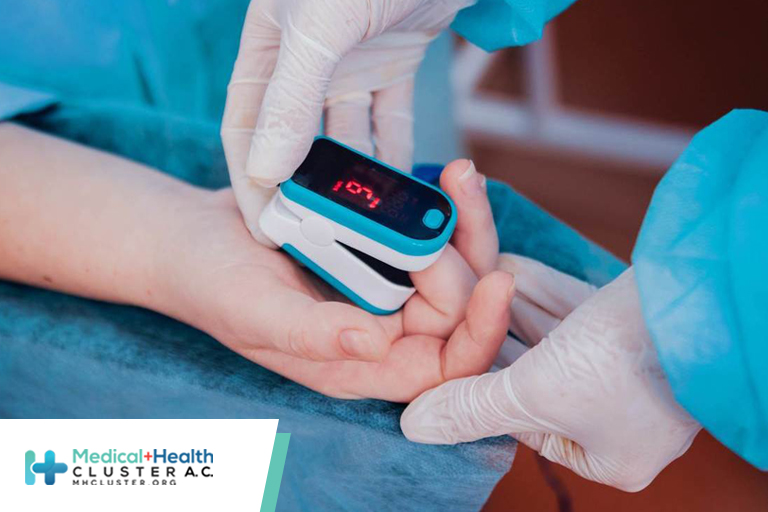
My first personal encounter with COVID-19 was with a 63-year-old friend residing in Kingston, the capital city of Jamaica. Her husband had recently died of complications of coronavirus infection, and the entire household was experiencing symptoms. I called to give my condolences and received a tearful account of the preceding week’s events. Her husband had an unusual headache that had been attributed to stress and an ear infection. Within a week, he became dyspneic and was admitted to hospital. Two days after his admission for COVID-19, he died.
On my second call with her, she expressed concern about having an unrelenting fever (now day 8). She casually mentioned that she had purchased a pulse oximeter and some vitamins based on information about COVID-19 on the internet. Nonchalantly, she asked, “How do you interpret the readings? I assume that if it is over 90%, it is good. My readings are between 90% and 92%. I can take deep breaths in, and I have no problem breathing.” I explained that an oxygen saturation below 94% requires an urgent care visit and that she may need medication, such as steroids and antibiotics. She refused admission despite her worsening dyspnea, and I advised her to contact her family doctor immediately. Her physician prescribed dexamethasone, azithromycin, and an expectorant.
A Far-Fetched Idea?
A home pulse oximeter is an inexpensive device that allows persons with severe COVID-19 to access care in a timely manner. Studies evaluating the use of home pulse oximetry in children in low-resource settings show that this simple tool can result in earlier diagnosis and reduced mortality from respiratory illnesses. In COVID-19 management, this is particularly true because of the prevalence of silent hypoxia (attributed to older age), comorbidities (eg, diabetes, which blunts the response to hypoxia), inherent variability of respiratory drive between persons, and a shift in the oxygen dissociation curve to the right with fever.
The World Health Organization (WHO) guidance on home care of persons with COVID-19 recommends monitoring for alarm symptoms as indicators of worsening illness and the need to seek urgent care. However, such symptoms as dyspnea, altered mentation, dizziness, and blue lips or face often occur after significant hypoxia is established. For example, 50% of persons discharged from an emergency department who subsequently recorded an oxygen saturation below 92% on home pulse oximetry did not report worsening symptoms. Therefore, home pulse oximetry is mentioned as an adjunct for home monitoring in the WHO guidelines; this aspect of home care has been neglected in low-resource settings, however.
Provision of home pulse oximetry in low-resource settings may seem far-fetched at first glance. Despite its low cost, pulse oximetry is often unavailable in health facilities in low-resource settings and exposes the challenge of supplying basic equipment for delivery of healthcare in these areas. A pulse oximeter costs 20-40 US dollars. Yet, a 2010 survey showed that 51%-70% of surgical theaters in low-income countries were not equipped with pulse oximeters. In a 2015 assessment of hospitals and facilities in northeast Haiti, none of the facilities had pulses oximeters; however, other point-of-care devices (eg, glucometers) are successfully used and have been incorporated into guidelines in low-resource settings.
Recently, the US Food and Drug Administration issued a warning about the inaccuracies of pulse oximetry in Black persons because racially diverse populations were not included in the development of these tools. Sjoding and colleagues at University of Michigan Medical School reported that occult hypoxemia occurred three times more frequently in Black patients (11.4%; 95% CI, 7.6% to 15.2%) than in White patients (3.6%; 95% CI, 2.5% to 4.6%), on the basis of paired arterial blood gas measurements and pulse oximetry. Although these findings are of concern and emphasize the need for validation in other populations, they do not negate the importance of pulse oximetry in low-resource settings with predominantly black populations.
First, there is limited access to arterial blood gas measurements in low- and middle-income countries, and pulse oximetry is often the only available tool for assessing oxygen saturation. Sjoding and colleagues also showed that the discrepancy between arterial blood gas measurements and pulse oximetry was greatest for oxygen saturations below the cutoff level that would act as a trigger for hospitalization. A 90% concordance between arterial blood gas measurement and pulse oximetry for patients with oxygen saturations between 92% and 96% confirms that pulse oximetry is a useful tool in a setting with few options for detecting hypoxia.
Second, pulse oximeter readings are not used in isolation but as another signal or indicator of severe COVID-19 disease, thereby increasing the sensitivity of the triage process. Besides, global interconnectivity results in unregulated access to pulse oximeters through local or online purchases as well as through family members residing in developed countries. Thus, home pulse oximetry in low-resource settings should not be ignored.
A Reminder and an Opportunity
The following weeks were harrowing for my family friend. She was diagnosed with COVID-19, and her dyspnea progressively worsened. In one telephone conversation, she exclaimed, “I cannot talk now. Pray for me!” Weeks after the onset of her symptoms, she continues to have occasional episodes of dyspnea, but her acute symptoms have resolved. She credits her survival to a casual conversation about a pulse oximeter reading, timely treatment, and fervent prayers.
She serves as a reminder that home pulse oximeter plays an important role in COVID-19 management and, despite its limitations, should not be overlooked in low-resource settings. At a minimum, all health facilities that triage patients with COVID-19 should have access to pulse oximeters. Moreover, the use of home pulse oximetry for high-risk persons with COVID-19 should be given serious consideration. Information should be available on preferred or validated devices, interpretation of readings, the limitations of the device, and when to seek medical advice. This simple tool should be included in the guidelines for home management of COVID-19 in low-resource settings where the options for reducing mortality are few. Otherwise, we will miss the opportunity to affect mortality at low cost.
Créditos: Comité científico Covid




