CONDENA MH CLÚSTER ATAQUE ARMADO A HOSPITAL ARCÁNGELES
Leer más
Clinical Trials Mix Vaccine Types to Boost COVID Protection
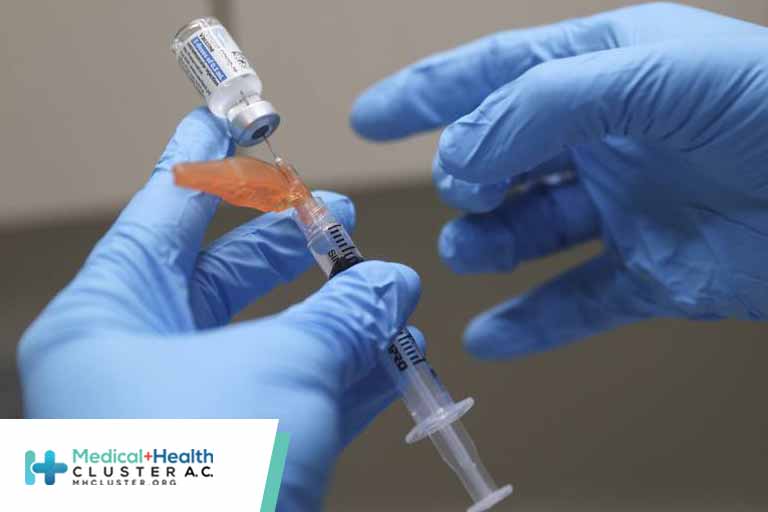
So far, the vaccines approved in the United States have been able to stand up to the most concerning SARS-CoV-2 mutations, but the fast-multiplying variants have investigators wondering whether a vaccine mix could help protect against unknown threats.

Ross Kedl
Combining different vaccine platforms — known as a heterologous prime-boost strategy — likely enhances immunity, according to Ross Kedl, PhD, from the University of Colorado in Aurora.
The strategy has been used in animal studies for decades, “and it is well known that this promotes a much better immune response than when immunizing with the same vaccine twice,” he told Medscape Medical News.
Effectiveness has also been shown in early human studies. An Ebola regimen that consisted of an adenovirus vector, similar to the AstraZeneca COVID vaccine, and a modified vaccinia virus vector showed promise in a phase 1 study. And an HIV regimen that consisted of the combination of a DNA vaccine, similar to the Pfizer and Moderna mRNA vaccines, and another viral vector vaccine showed encouraging results in a proof-of-concept study.

John Moore
In fact, the heterologous prime-boost concept has been used in HIV trials for 25 years, said John Moore, PhD, from Weill Cornell Medical College in New York City, whose background before the pandemic was in HIV research.
There’s plenty of evidence to show that mixing these platforms is safe, he said, but in the case of HIV, “it hasn’t proved beneficial.”
That problem lies more with the complexity of HIV than with failed research. “The reason HIV vaccines don’t work and COVID vaccines do,” Moore explained, “is that HIV is incredibly hard to vaccinate against, whereas for COVID, it turns out, it’s quite straightforward.”
In the HIV field, the most common strategy is to prime with a viral vector, like adenovirus, and then to boost with a protein or DNA. There have been very few HIV mRNA trials to date because the technology is so new.
But “there is plenty of evidence that these strategies make sense” for COVID-19, he pointed out. It is possible that a prime-boost would increase efficacy, “but the only way to do that is to get safety data and then efficacy data.”
A Strong Vaccine Cocktail
One such trial — the first of its kind — is underway in the United Kingdom, where researchers are examining immune responses in patients who receive one dose of the Pfizer mRNA vaccine followed by one dose of AstraZeneca adenovirus viral vector vaccine, or vice versa, at intervals of 4 and 12 weeks.
Another trial is testing the AstraZeneca adenovirus viral vector vaccine in combination with Russia’s Sputnik V, another viral vector vaccine.
Results from both trials are expected in about 2 months, and could provide clues for those who want to mix vaccines other than those being tested.
In general, a stronger antibody response increases the body’s ability to deal with more resistant variants.
“Suppose an mRNA vaccine was followed by a protein vaccine, like Novovax, and that gave a substantial increase in antibody titers. That increase would be beneficial in dealing with variants. We don’t know this, but it’s a sensible thing to try,” Moore said.
However, he warned, no one should try to get a mix of shots on their own.
Guidance from the Centers for Disease Control and Prevention says that vaccines “are not interchangeable,” and cautions that the administration of two doses from different vaccine manufacturers should be done only in “exceptional situations.”
CDC Warns Against Mixing
“There are absolutely no safety reasons to think mixing would be a problem,” Moore said, “but there’s no guidance or data on heterologous boost.”

Buddy Creech
And currently, there’s no pressing need to make the three vaccines approved for emergency use in the United States work better, said Buddy Creech, MD, MPH, director of the Vanderbilt Vaccine Research Program in Nashville, Tennessee.
All three approved vaccines — Pfizer, Moderna, and Johnson & Johnson — are nearly 100% effective at preventing hospitalization and death due to COVID-19, he added.
“We may learn that there is a slight difference in the durability of the response among them,” Creech said, but “we haven’t yet.”
Still, there are reasons to test vaccine combinations: to increase flexibility in the global vaccine supply; to provide a backup for people who find they are allergic to a particular vaccine; and to provide protection against a particular mutated virus.
Trials will also test combinations of existing vaccines with versions from the same manufacturer tweaked to fight particular variants.
The phase 1 trial of a new Moderna vaccine that targets the B.1.351 South African variant was announced last week. Researchers will be evaluating different combinations — the original vaccine with a variant booster, the variant vaccine followed by a variant booster, and a half-and-half mix of the original and variant vaccines for both doses — said Creech, who is one of the trial’s principal investigators.
Mixes could happen across platforms, as well, he said. If someone got a J&J shot and a variant erupted, it would be easier to make an mRNA vaccine against the variant. A reasonable approach would be to boost a J&J shot with a Moderna or Pfizer vaccine developed to target that variant.
“It would be nice to understand and define what it looks like to have gotten dosed with the J&J and then boosted with another,” he said.
However, there doesn’t seem to be an inherent biologic advantage to mixing vaccines from different platforms, Creech said.
“Basically, when we turn your muscle cell into the manufacturing plant for this vaccine, we generate phenomenal vaccine responses and we generate fantastic immunity while having a very favorable side-effect profile,” he said.
The end goal is the same for both mRNA and viral vector vaccines: vaccinated people will make the spike protein in their muscle. That spike protein will look the same because the vaccines start with the same genetic sequence.
But, Creech asked, “is there any advantage to delivering that sequence in a fat bubble — the lipid nanoparticle with the mRNA vaccine — or as an unrelated virus, like adenovirus in the viral vector vaccines? We simply don’t know yet if one has an advantage over the other.”
For now, the field of COVID-19 vaccines is seeing “a lot of contingency planning,” whether or not people will need different products or boosters or a vaccine for a particular variant, he explained.
“We’ve seen this happen with influenza,” he said. “Every year, you don’t remember what brand of vaccine you got last year. It’s because we’ve built in these contingencies. Each year there will be plenty of flu vaccine, but we don’t know which manufacturer will make the most. We may have to get to that point with COVID.”
In a couple of months, interim trial results should help establish whether combinations of vaccines from different platforms are effective.
“Ideally, we would have started this last year, but the priorities were different,” said Moore. “The priority was to get vaccines tested and to get them out there. We’re in a different phase now, where you can put some planning in and set things up for the next generation of experiments.”
Marcia Frellick is a freelance journalist based in Chicago. She has previously written for the Chicago Tribune, Science News and Nurse.com and was an editor at the Chicago Sun-Times, the Cincinnati Enquirer, and the St. Cloud (Minnesota) Times. Follow her on Twitter at @mfrellick.
Créditos: Comité científico Covid




